Scroll to:
Organization and performance indicators of the emergency department in the children's clinic in the city of Ufa
https://doi.org/10.21886/2219-8075-2024-15-2-112-116
Abstract
The article presents the work experience and retrospective analysis of the indicators of the emergency department for children of the "Children's Clinic No. 5" in Ufa for 2023. The average number of calls to emergency services was 3491 calls per year. On average, one doctor in the department handles 10–12 calls per day. However, throughout the year there is an uneven load on the emergency department: in the autumn-winter period the frequency of calls increases to 20–30, in the summer months it decreases to 3–5 calls. The overwhelming majority of calls were made by those aged 3–7 years (35% of cases); teenagers sought emergency help least often (6% of cases). The largest percentage of visits was due to hyperthermic syndrome (43% of cases), obstruction of the upper and lower respiratory tract was recorded in second place (21% of cases), and calls related to pain syndrome were in third place (12%). Analysis of the morbidity structure by nosology demonstrated the following results: the leading pathology (70,2% of cases) was acute respiratory viral infection, the second place was occupied by diseases of the gastrointestinal tract (15,5% of cases). Thus the emergency medical care department contributes to the timely and effective provision of emergency care to children at home, prevents the development of decompensation of body functions, reduces the risk of disability and promotes the health of young citizens of the Russian Federation.
For citations:
Tikhonova R.Z., Yakovleva L.V., Mursalimov V.D. Organization and performance indicators of the emergency department in the children's clinic in the city of Ufa. Medical Herald of the South of Russia. 2024;15(2):112-116. (In Russ.) https://doi.org/10.21886/2219-8075-2024-15-2-112-116
For decades, providing emergency medical care to children in life-threatening situations continues to be the most pressing and socially significant issue in pediatrics [1]. As a rule, children are susceptible to more severe development of life-threatening conditions, due to anatomical and physiological characteristics of their body, immaturity of tissue and cellular structures, and imperfection of the neurohumoral regulation of organs and systems; sometimes these are burdened obstetric and genealogical history [2].
Timely and comprehensive emergency care contributes to a more rapid and adequate functioning of the compensatory mechanisms of the child's body during the pathological process, reduces the duration of therapy received in the hospital, and decreases adverse disease outcomes and the level of disability in children.
The conducted statistical analysis indicates an annual increase in life-threatening situations in children. Therefore, the key points in providing emergency care to the pediatric population are the following: early initiation, a stage-by-stage approach, and continuity of medical care [3][4].
The main goal of providing emergency care to a child at the pre-hospital stage is using the minimum amount of necessary manipulations aimed to preserve and maintain the most significant life-support functions. The pediatrician of the emergency medical care department (EMCD) faces the following fundamental tasks: conducting a diagnostic search for a condition that threatens the life and health of the patient; providing the necessary set of emergency care techniques; and making a decision on further routing [5]. After the initial examination, the pediatrician must identify the main prognostically unfavorable syndrome and/or establish a nosological diagnosis, assess the severity of the patient's condition, and determine the emergency medical measures and the optimal administration of drugs. The initial assessment of a threatening condition includes the identification of signs of decompensation of the respiratory system, blood circulation, and the degree of depression of the central nervous system (CNS) [6]. When assessing the work of the CNS, the presence or absence of consciousness and the reaction to a painful stimulus are taken into account; the width of the pupils and their reaction to light, the adequacy of muscle tone, and the occurrence of clonic or tonic seizures are recorded. When assessing the work of the respiratory system, attention is paid to the presence/absence of breathing, bradypnea, the type of pathological breathing, signs of dyspnea (difficulty inhaling or exhaling, mixed dyspnea, pallor, cyanosis, nose flaring, participation of accessory muscles in the act of breathing). When examining the state of blood circulation, central hemodynamics are assessed, namely, pulse (frequency, rhythm, filling, conduction to the periphery), systemic arterial blood pressure, and examination of peripheral blood flow by skin color (pallor, prevalence of cyanosis, marbling) [7]. Collecting anamnesis of the disease is of no small importance, but the difficulty lies in the fact that the pediatrician has a limited time to obtain the necessary information. Therefore, at the first stage, it is necessary to obtain information about the causes of a threatening condition, assess the strength and impact duration of unfavorable factors on the prognosis of the disease, assess the anamnesis (complicated pregnancy and childbirth, intrauterine hypoxia, concomitant chronic pathology, allergic reactions to food, drugs, vaccine administration, etc.).
Undoubtedly, young children, as a rule, need urgent emergency medical care, since they experience decompensation of vital functions of the body quite quickly. In this regard, the key issue in ensuring and maintaining the health of the younger generation at a high level is the development and improvement of emergency care in the outpatient sector of health care. Thus, the Order of the Ministry of Health and Social Development of the Russian Federation dated April 16, 2012 No. 366n “On approval of the Procedure for provision of pediatric care” recommends creating an EMCD in the structure of a children's polyclinic, which should provide for 2 positions of a pediatrician of the EMCD per 10,000 assigned children and 2 positions of a pediatrician nurse1. The fundamental objective of organizing such a department on the basis of a polyclinic is a proportionate reduction in the load on emergency medical care, and coordination in the work of doctors of the EMCD and district pediatricians, since, despite modern diagnostic methods and algorithms for providing emergency care to children, pediatricians are not always ready to quickly apply certain algorithms of actions included in modern standards of medical care that meet the requirements of high efficiency and safety.
In the structure of the State Budgetary Healthcare Institution of the Republic of Bashkortostan “Children's Polyclinic No. 5” of Ufa, an EMCD was organized aiming to provide primary health care in case of sudden acute diseases, conditions, and exacerbation of chronic diseases that are non-life-threatening and do not require emergency medical care. The department began its work in April 2009; its work schedule was in accordance with the State Guarantees Program, constituting a twelve-hour period – 8 AM – 8 PM on weekdays and 8 AM – PM on Saturdays. Calls are accepted until 7 PM from Monday to Friday and until 4 PM on Saturday. Each call is entered into the registration log for emergency medical care for children, indicating the date and time of its receipt, patient data, and reason for the call; a “Call Card” is filled in.
The mobile emergency medical care team is staffed by a pediatrician and a nurse, as well as a driver. To date, documents regulating the medical kit for providing emergency care by a pediatrician are absent; therefore, the authors of the present study directly developed the necessary set of devices (portable nebulizer and electrocardiograph, glucometer with test strips, tonometer, stethoscope, pulse oximeter, oropharyngeal airway), drugs (antipyretics, antispasmodics, bronchodilators, antiallergic, hormonal analeptics), dressings, and antiseptics.
The emergency medical care physicians have completed a training course, including lectures and practical classes using simulators at the multidisciplinary accreditation and simulation center of the Bashkir State Medical University, and have acquired a set of fundamental knowledge and key skills in basic cardiopulmonary resuscitation [8]. The clinic developed standardized algorithms for providing emergency care at the outpatient stage for various emergency conditions (hyperthermia, anaphylactic shock, obstructive syndrome, foreign body aspiration, etc.).
After conducting the necessary emergency therapy, the emergency medical care pediatrician draws up an examination report in electronic format. The severity of the child's condition, the diagnostics performed, and the range of emergency measures and their effectiveness are noted, and appropriate recommendations are given. All the information on the child (underlying disease, comorbid pathology, severity of exacerbation of the disease, emergency measures taken) is transferred to the supervising district pediatrician for further monitoring of the child's condition; if necessary, basic therapy is adjusted, and if the condition worsens, the patient is hospitalized. Information about complex cases and non-standard situations is immediately transferred to the head of the EMCD for making a decision on further actions.
In accordance with the objectives, a retrospective analysis of the performance indicators of the EMCD in the State Budgetary Healthcare Institution of the Republic of Bashkortostan “Children's Polyclinic No. 5” in Ufa for 2023 was carried out. The average number of calls to the emergency service was 3491 per year. At the same time, calls in 2023 increased by 1.4 times compared to 2019 and by 1.8 times compared to 2020; this may be due to the increase in the new coronavirus infection in the pediatric population.
The authors of the present study found that on average, one medic of the department handled 10–12 calls per day. Analysis of the work of the emergency medical service showed that the workload of the department was uneven throughout the year. Thus, in the autumn-winter period, the frequency of incoming calls increased by 2–3 times and reached 20–30, in the summer months, as a rule, it decreased to 3–5 calls. The current situation may be associated with an increase in respiratory viral infections among children. In the autumn-winter period, the circulation of viruses and their resistance to low temperatures increase; children spend less time outdoors due to weather conditions, which leads to crowding in children's social groups; microbiocenosis of the respiratory tract mucous membranes is disrupted due to the deterioration of microecology (decreased absolute humidity of the outside air and dryness of the indoors air), and suppression of various links of the immune system by viruses. All these factors facilitate easier penetration of viruses through the epithelium of the upper respiratory tract and an increase in morbidity.
An analysis of the distribution of calls received by the emergency medical service by hours showed that the main workload fell on the morning hours (from 8:00 to 12:00), amounting to 46%; second was servicing patients with emergency conditions from 12:00 to 17:00 (34.8%). The fewest calls (19.2%) fell on the evening hours (from 17:00 to 20:00). Patients under three years of age, regardless of the reason for contacting, when calling the lines 03, 103, and 112 are served by an ambulance team.
The present analysis of the age of patients seeking emergency medical care revealed the following: the greatest number of calls was for those aged 3–7 (35% of cases). This may be due to the fact that a large proportion of children begin to attend preschool institutions where they experience increased contact with a wide range of different pathogens against the background of the development of the body's immune system, increased susceptibility to infectious agents, and the development of allergic pathology in some patients. Next was the category of children aged 1–3 (23% of cases) and 7–14 (21% of cases). Adolescents aged 14–18 sought emergency care the least often (6% of cases). Most likely, this is due to maximalist views, an unfounded assessment of the health level, and a distorted definition of the physical condition of the body as a whole.
Of the children served through emergency care, almost an equal proportion was transferred to home observation by a local pediatrician (45% of patients) or invited to an outpatient appointment (54% of patients). Only about 1% of children were hospitalized in city hospitals. The obtained data indicate a significant contribution and positive trends in the work of the emergency medical service in providing emergency care to the pediatric population, which in turn reduces the burden on city hospitals and indicates a sufficiently high professional level of training and technical equipment of the medical team providing emergency care at home.
The assessment of the reasons for contacting the emergency medical service showed that the largest share fell on hyperthermic syndrome, which was 43% of all calls serviced; the second was obstruction of the upper and lower respiratory tract (21% of cases), and the third was pain syndrome of various localizations (12% of calls). About 6% of cases of the emergency medical service team’s visits to patients were classified as “other reasons”, associated with the class of “injuries, poisoning and some other consequences of exposure to external causes” (Fig. 1).
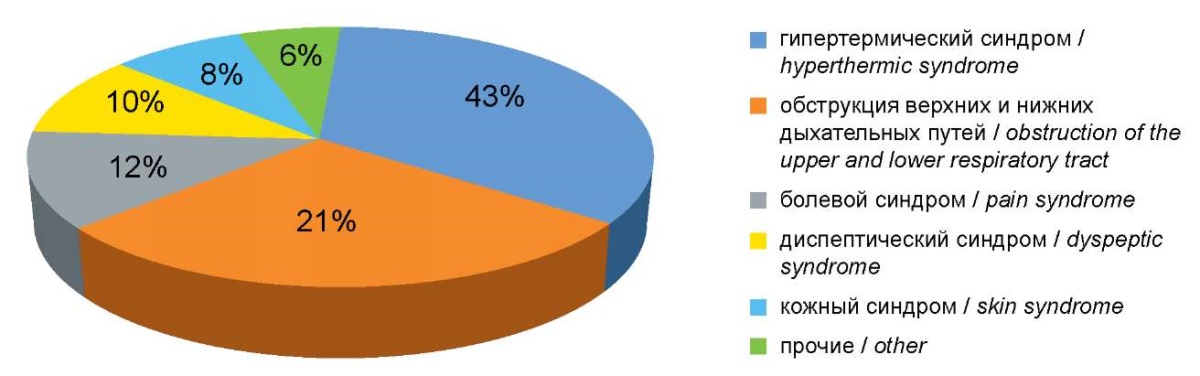
Рисунок 1. Структура причин обращения в ОНМП.
Figure 1. Structure of reasons for contacting emergency departments.
Analysis of morbidity by nosology demonstrated the following: the leading pathology, occupying more than 70.2%, is acute respiratory viral infection, second are diseases of the gastrointestinal tract – 15.5% (Fig. 2).
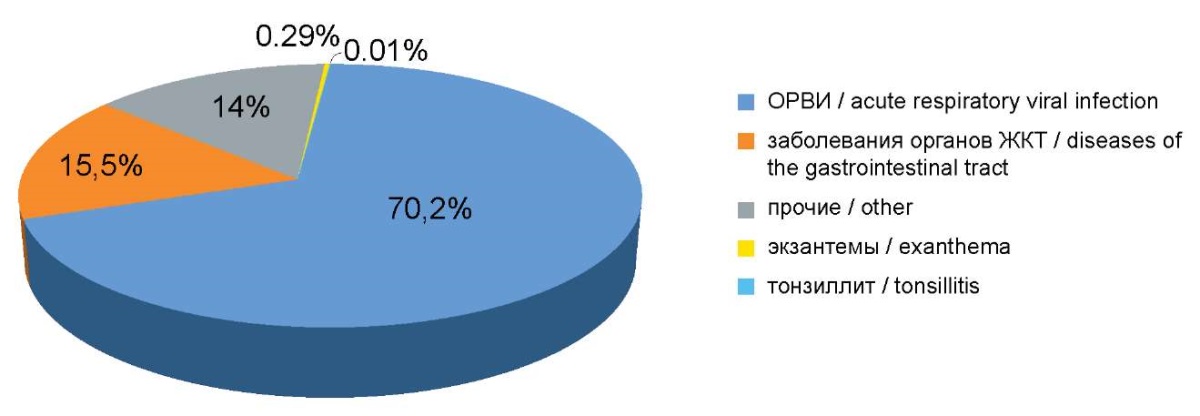
Рисунок 2. Структура заболеваемости по нозологии в ОНМП.
Figure 2. Morbidity structure by nosology emergency departments.
Thus, organizing emergency medical care in the structure of the State Budgetary Healthcare Institution of the Republic of Bashkortostan “Children's Polyclinic No. 5” in Ufa laid the foundation for developing emergency care for the city's children. Notably, the availability of an accessible material and technical base and the qualifications and professionalism of the emergency medical care staff contribute to the most timely and effective provision of emergency care at home. This ensures the effectiveness of subsequent treatment, prevents decompensation of body functions, and reduces the risk of loss of working capacity, which contributes to the overall strengthening of the health of young citizens of the Russian Federation.
1. Order of the Ministry of Health and Social Development of the RF dated April 16, 2012 No. 366n “On approval of the Procedure for provision of pediatric care”. https://www.consultant.ru/document/cons_doc_LAW_130620/
References
1. Choloyan S.B., Pavlovskaya O.G., Sheenkova M.V., Pavlenko L.I. Twenty years of experience of emergency medical service at the city child hospital. The Bulletin of Contemporary Clinical Medicine. 2018;11(6):52-56. (In Russ.) https://doi.org/10.20969/vskm.2018.11(6).52-56
2. Baranov A.A., Albitskiy V.Y. State of health of children in Russia, priorities of its preservation and improving. Kazan medical journal. 2018;99(4):698-705. (In Russ.) https://doi.org/10.17816/KMJ2018-698.
3. Zhdanova L.A., Runova O.S., Postol I.I., Shishova A.V. Immediate medical care organization in municipal pediatric polyclinic. Bulletin of the Ivanovo State Medical Academy. 2015;20(2):5-9. (In Russ.) eLIBRARY ID: 24094801 EDN: UHGXZD
4. Moskvicheva M.G., Shchepilina E.S. Analysis of heads of medical organizations and medical stuff opinions on emergency medical care organization. Meditsinskoe obrazovanie i professional'noe razvitie [Medical Education and Professional Development]. 2019;10(4):84-93. (in Russ.) https://doi.org/10.24411/2220-8453-2019-14006 .
5. Choloyan S.B., Pavlovskaya O.G., Ekimov A.K., Sheenkova M.V., Tricomenas N.N., et al. Modern approaches to the analysis of emergency medical care for children. Manager zdravoohranenia. 2019;(9):9-22. (In Russ.) eLIBRARY ID: 41316451 EDN: CTMJOR
6. Choloyan S.B., Pavlovskaya O.G., Sheenkova M.V., Baigazina E.N. The place of a medical information system in providing medical care to children. Russian Bulletin of Perinatology and Pediatrics. 2018;63(4):152–153. (In Russ.). eLIBRARY ID: 35510248 EDN: XXRBQD
7. Starec E.A., Kotova N.V., Loseva E.A., Fedorenko O.V. Simulation training in pediatrics and neonatology: assessment, recognition and stabilization of pediatric emergencies. Child's health. 2018;13(4):405-409. (In Russ.). eLIBRARY ID: 35259567 EDN: XTGYZN
8. Yakovleva L.V. Shangareeva G.N., Yumalin S.Kh. Experience in the use of simulation technologies in the preparation of primary specialized accreditation in the specialty "Pediatric Cardiology". Bulletin of the Bashkir State Medical University. 2022;7:121-126. (In Russ.) eLIBRARY ID: 50162569 EDN: GNAWUT
About the Authors
R. Z. TikhonovaРоссия
Lyudmila V. Yakovleva - Dr.Sci. (Med.), Professor, head of Department of polyclinic and emergency pediatrics with the course of Institute of Additional Professional Education.
Ufa
Competing Interests:
Authors declares no conflict of interest
L. V. Yakovleva
Россия
Regina Z. Tikhonova - Candidate of Medical Sciences, аssistant professor of Department of polyclinic and emergency pediatrics with the course of Institute of Additional Professional Education.
Ufa
Competing Interests:
Authors declares no conflict of interest
V. D. Mursalimov
Россия
Valery D. Mursalimov - аssistant Department of polyclinic and emergency pediatrics with the course of Institute of Additional Professional Education.
Ufa
Competing Interests:
Authors declares no conflict of interest
Review
For citations:
Tikhonova R.Z., Yakovleva L.V., Mursalimov V.D. Organization and performance indicators of the emergency department in the children's clinic in the city of Ufa. Medical Herald of the South of Russia. 2024;15(2):112-116. (In Russ.) https://doi.org/10.21886/2219-8075-2024-15-2-112-116
JATS XML







































